San Francisco Is Giving Pregnant
Black & Pacific Islander Women
$1,000 A Month
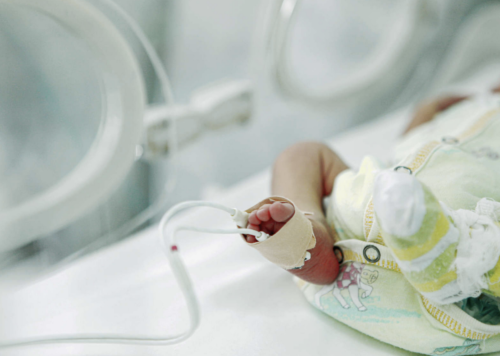
Rates of premature births & infant mortality are significantly higher for women of color compared to white women, and the new supplement is designed to narrow racial & financial disparities among expectant mothers.
By Ashleigh Carter, Now This, Sept. 16, 2020
https://nowthisnews.com/news/san-francisco-gives-black-pacific-islander-moms-1000-a-month
San Francisco is launching a new program that will provide monthly financial assistance to Black and Pacific Islander expecting moms.
On Monday, San Francisco Mayor London Breed announced the new pilot program called The Abundant Birth Project. The program will provide $1,000 a month to pregnant Black and Pacific Islander women through the duration of their pregnancy and for six months after they give birth.
150 women will be chosen to receive the monthly supplement, and the project will work closely with the city’s “pregnancy support services” to determine who will be eligible to receive the money. The project organizers hope to expand and provide the monthly payments for up to two years after the baby is born.
Mayor Breed said the supplemental income will help expectant mothers “put their health first” when they normally wouldn’t because of financial restraints.
Prematurity is one of the leading causes of infant mortality in the U.S., according to the March of Dimes. Breed’s office said prematurity is also linked to behavioral developmental issues, learning difficulties, and chronic diseases. The office also said that in San Francisco,
“Black infants are almost twice as likely to be born prematurely compared with white infants,” and “Pacific Islander infants have the second-highest preterm birth rate.”
According to the Centers For Disease Control and Prevention, Black and Indigenous women are three times more likely to die from a pregnancy-related cause than white women in the U.S.
“Structural racism, which has left Black and Pacific Islander communities particularly exposed to COVID-19, also threatens the lives of Black and PI mothers and babies,” San Francisco pediatrician Dr. Zea Malawa said in a statement. “It is exciting to be in a city that not only calls out racism as a problem, but also takes steps to heal the wounds left by decades of injustice and anti-Black sentiment.”
The Abundant Birth Project is in partnership with Expecting Justice, a Black woman-led nonprofit that works to provide care and financial assistance for Black and Pacific Islander mothers in the San Francisco area.
The organization also focuses on the racial disparities Black and PI women face while pregnant and works to “ensure safe and healthy childbirth.”
“The Abundant Birth Project is rooted in racial justice and recognizes that Black and Pacific Islander mothers suffer disparate health impacts, in part because of the persistent wealth and income gap,” said Breed.
BC Nurses and Physicians Can Now
Prescribe Alternatives to Street Drugs

Daily Hive Vancouver Staff, Sept. 16, 2020
https://dailyhive.com/vancouver/dr-bonnie-henry-public-health-order-overdose
In an effort to slow the overdose crisis and ultimately save lives, BC’s Provincial Health Officer Dr. Bonnie Henry issued a public health Wednesday morning to increase the number of health professionals authorized to help people at risk for overdoses access safer alternatives to the toxic street drug supply.
The order, issued under the Health Professions Act, authorizes registered nurses and registered psychiatric nurses to prescribe pharmaceutical alternatives to street drugs to help separate more people from the poisoned street drug supply to save lives and provide opportunities for ongoing care, treatment and support.
New nursing standards will also be introduced, along with training and education, and access to expert consultation and pathways to connect people to broader addictions and primary care.
“We know the pandemic has only made the street drug supply in B.C. more toxic than ever, putting people who use drugs at extremely high risk for overdose,” Henry said.
“Giving physicians and nurse practitioners the ability to prescribe safer pharmaceutical alternatives has been critical to saving lives and linking more people to treatment and other health and social services”
Henry said she is issuing the order:
“to expand the health professionals who are able to provide safer, accessible alternatives to the toxic street drug supply and help more people find their pathway to hope.”
In addition to the public health order, the Ministry of Mental Health and Addictions and the Ministry of Health are working with the Office of the Provincial Health Officer to develop an updated policy directive for prescribers and health authorities, which builds on the existing risk mitigation clinical guidance released in March 2020 in partnership with the BC Centre on Substance Use.
“Before the COVID-19 pandemic began, B.C. was making progress and overdose deaths were coming down for the first time since 2012,” said Judy Darcy, Minister of Mental Health and Addictions.
“We’re seeing these tragic spikes in deaths across Canada, but I’m proud that we’re the only government responding across the full continuum of care by providing more overdose prevention services and outreach teams, doubling youth treatment beds, increasing adult beds and counselling services.”
The policy directive is being urgently finalized and is expected to be released as soon as possible in order to:
- Expand eligibility criteria to prioritize reducing overdose events and deaths, and reach individuals with opioid-use disorder, other substance-use disorders or individuals with a history of accessing the toxic street drug supply who are at high risk of overdose and other drug-related harms;
- Carefully expand the types of medications that can be prescribed and dispensed by doctors, pharmacists and nurses;
- Increase access points to allow for dispensing medications from health authorities and community pharmacies;
- Continue to commit to ongoing evaluation and monitoring and support evidence-based care planning.
In addition to the public health order, the Ministry of Mental Health and Addictions and the Ministry of Health are working with the Office of the Provincial Health Officer to develop an updated policy directive for prescribers and health authorities, which builds on the existing risk mitigation clinical guidance released in March 2020 in partnership with the BC Centre on Substance Use.
Meet the Cyclist Squad
Saving Lives in the Downtown Eastside

DTES Bike Squad paramedics Tom Venables (left), Troy Gienger, Chris Iregui, and Darren Metta Photo: BCEHS
DTES bike paramedics responded to 63 emergency calls in their first 10 days.
By Sarah Grochowski, Vancouver Is Awesome, Sept. 17, 2020
After nearly a year away from their bicycles, four Downtown Eastside paramedics have returned to two wheels.
When BC Emergency Health Services Bike Squad was reinstated Sept. 4, its DTES members attended 63 medical emergencies in just ten days.
Calls they responded to covered almost 20 per cent of Vancouver overdose calls in that same timespan, said BCEHS paramedic Darren Metta, one of the riders.
The 50-year-old gears up at 9 a.m. four days a week for a 45-kilometre ride that sees him and his partner work to save lives 11 hours straight.
For people in the DTES community, Bike Squad members offer a friendly face without the attention that ambulance sirens draw to a person suffering a medical emergency.
“We get flagged down a lot,” Metta elaborated.
“People walk up to us. A lot of times they don’t have access to a phone and tell us about someone nearby who ‘doesn’t look so good’,” he said.
“Then we’ll go check it out and they won’t need to call 911.”
It’s been four years since the BCEHS program first touched down in the neighbourhood.
Last year, from May 1 to Oct. 31, the team prevented 1,064 ambulance calls in downtown Vancouver due to their on-scene care.

This year, the COVID-19 pandemic has posed a unique challenge to the paramedics, who work to dismount their bicycles at a safe social distance while being approached for help.
For every call, the paramedics don personal protective gear including a face shield, mask, and gloves. When there is a suspected COVID-19 case, the attendants wear a full-body gown.
“A lot of times we can get to the scene first,” Metta explained, as bikes can navigate congested areas and arrive at the patient’s side faster than a traditional ambulance.
“It often reduces the time it takes for the person to get treated.”
And in instances of overdose, heart attack, or life-threatening injuries, every second a paramedic saves counts, said BCEHS spokesperson Sarah Morris.
“We also carry all the same medical equipment inside an ambulance, except for the stretcher,” Metta remarked.
The gear adds an extra 50 pounds to their mountain bikes, which are fitted with purpose-built panniers.
Though it’s not always an easy job, Metta said it is a deeply rewarding one.
As a paramedic for the last 20 years, he has preferred interacting with the DTES community from the seat of his bike.
The BCEHS Bike Squad will be deployed until Oct. 31 as one of the several fleets in communities around B.C., including the Vancouver International Airport.

